Introduction
The overprojected nasal tip, commonly referred to as the “Pinocchio” nose, is a relatively uncommon but challenging deformity.1 Surgical correction of the nasal tip is most difficult and the least predictable component of rhinoplasty surgery The goal of the nasal aesthetic surgeon is to use his or her judgment to try and achieve the patient’s goals and optimize the aesthetics of the nose.
Nasal tip projection is important for both aesthetic and functional reasons. It is important from a cosmetic point for facial harmony but also functionally for adequate air entry. The patient’s aesthetic goal must be carefully balanced with the maintenance of functional support since any procedure that reduces tip projection narrows the nasal valve and reduces air flow. Aside from the nasal anatomy, the perception of nasal tip projection is influenced by many factors. These include chin projection, upper lip height, nasolabial angle, dorsal height, nasofrontal angle and other physical characteristics.2
Nasal tip support has been classified into two categories, major and minor groups. Major tip-support mechanisms were first described by Janeke and Wright which have been further studied.3 The “tripod concept” was then described, which relates the medial and lateral crura to projection and rotation of the nasal tip.4,5 This emphasized the importance of the extensive ligamentous attachments between the crural cartilages.5,6,7 Generally, major tip support includes (1) the size, shape and resiliency of medial and lateral crura, (2) the attachment of the medial crural footplates to the caudal septum, and (3) soft-tissue attachment of the caudal margin of the upper lateral cartilages to the cephalic margin of the lower lateral cartilages.2,6 In addition, there are several minor tip-support mechanisms have been described, which include, the dorsal cartilaginous septum, the interdomal ligaments, the membranous septum, the nasal spine , the surrounding skin and soft tissues and the alar side walls.2,6
There are several definitions used to describe nasal tip projection. Essentially, it is a perpendicular measurement from the tip defining points to the nasal-alar crease.8
A number of methods have been described for the measurement of nasal tip projection. Methods have been described by Simons, Baum and Powell.9,10 Another method commonly used is Goodes’ analysis which states that when the nasofacial angle is between 36 and 40 degrees, the length of the perpendicular line through the tip defining point will be 0.55 to 0.60 of the length of the nasal dorsum.10
The overprojected nasal tip is a result of an excessive overgrowth of the lower half of the nose.1 The overdevelopment of anatomical components include the alar cartilage, septal cartilage, and nasal spine.11 However, the deficiency of adjacent structures involving the nasofrontal angle, saddle-nose deformity or mandibular retrusion or anterior displacement of the maxilla may also contribute to an overprojected nasal tip.
Several techniques of deprojecting the nasal tip have been described. This can be achieved by using techniques that can destroy the supports of the tripod or by shortening the legs with disruption of the ligaments connecting the medial ends of the lateral crura.7 Certainly, many techniques which are used involve weakening, dividing or excising segments of the alar area.11 Other less destructive techniques include releasing fibrous attachments, using either the delivery approach or a full or complete transfixion incision.11 A full transfixion incision disrupts the attachment of the medial crura to the caudal septum, with weakens the nasal tip support, resulting in deprojection of the tip. Although this concept has been described well in the literature and studied in conjunction with other tip deprojecting maneuvers, there have been no studies that have isolated the effect of the full transfixion incision alone.
The purpose of our study was to determine the effect of the full transfixion incision on tip projection. Specifically, two questions we addressed with this study were: (1) What is the quantitative effect of a full transfixion incision alone on nasal tip projection, and (2) Is there a difference in effect between different nasal skin types.
Methods
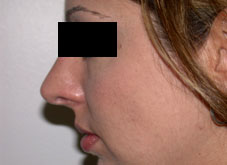
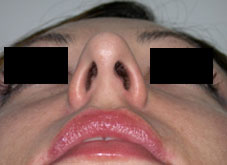
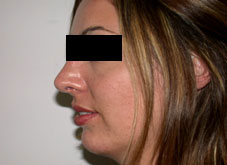
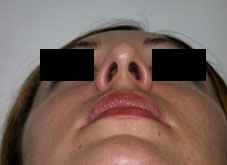
Seventy-two consecutive patients requesting primary septorhinoplasty procedures were enrolled in the study between January 2003 and February 2004. Patients were included if part of the patient’s aesthetic goal was a desire to reduce their nasal tip projection and were subjectively evaluated by the authors (R.R. or P.S.) to have an overprojected tip. Patients were excluded if revision procedures were requested. Tip projection was measured from the alar crease to the most prominent point of the nasal tip. Measurements were taken with calipers. The tip was considered projected if tip projection was greater than 2/3 of the length of the nose as a measurement from the nasion to the tip-defining point. Subjects were also categorized into three groups based on the quality of the skin, either thin, medium or thick skin based on the surgeon’s subjective analysis. Nasal tip projection measurements were performed preoperatively and immediately following the full transfixion incision.
All surgical procedures were performed by the authors (R.R. or P.S). No local anaesthetic was administered prior to the measurements or the incision. The full transfixion incision was fully taken down the membranous columella to the nasal spine, disrupting the fibrous attachments between the medial crura footplates and the caudal septum.
After measurements were taken, the remainder of the rhinoplasty was performed using the graduated approach. The graduated approach refers to the technique where one first reduces the forces extrinsic to the lower lateral cartilages that are projecting them away from the face before actually making changes to the lower lateral cartilages themselves.
Consent was obtained from each subject prior to entering the study.
Results
A total of 73 patients were enrolled in the study, comprising of 49 women (67%) and 24 men (33%). The average age was 27, ranging from 16 to 55 years of age.
The nasal tip projection was measured in millimeters (mm). Measurements were taken before and immediately after the full transfixion incision was performed and the difference between the two measurements was calculated for each patient. The overall mean nasal tip deprojection of all 73 patients after a full transfixion incision was performed was 1.6 mm, ranging from 0 to 3 mm (figure 1).
The patients were placed into one of three nasal skin thickness types: thin, medium and thick. There were 26 patients in the thin group, 30 patients in the medium group, and 17 patients in the thick group. The mean difference in each group was calculated. (Table 1) Patients with thin skin had a mean deprojection of 2.12 mm (S.D. 0.065). The mean nasal tip deprojection of patients with medium skin thickness was 1.3 mm (S.D. 0.065). For patients with thick skin, the mean nasal tip deprojection was 1.4 mm (S.D. 0.050). Overall, patients in the thin skin group had the greatest deprojection from the full transfixion incision compared to the other two groups.
To evaluate if the differences between the groups were statistically significant, a one-way ANOVA was performed. With an F-value of 13.173, it revealed that there was a significant difference in the mean deprojection among the three groups (Sig < 0.0005). To further identify which groups were significantly different, a post-hoc analysis was performed. (Table 2) A significant difference between the mean result of the thin skin group compared to both the medium skin and thick skin thickness groups. The difference in deprojection between the medium and thick skin group was not statistically significant. Therefore, not only did the thin skin thickness group have the largest deprojection of the nasal tip with the full transfixion incision, but that this was a significant difference compared to the medium and thick skin groups.
Discussion
The overprojected nasal tip continues to be a challenge to the rhinoplasty surgeon. It has only been in the last 40 years that we have understood the important components of nasal tip support which contribute to nasal tip projection. One of these components is the medial crura and their attachment to the caudal septum.12
There have been several techniques which describe methods to deproject the nasal tip. These techniques include the release of fibrous attachments, decreasing the volume of overdeveloped anatomic components, and repositioning the medial or lateral crura.11 Other methods have been described which give the illusion of a reduced nasal tip by deemphasizing nasal projection through the augmentation of adjacent structures.11
The full or complete transfixion incision is one method of releasing the fibrous attachments to deproject the nasal tip. The medial crura attachment to the caudal septum was identified in 1971 as an important component of nasal tip support.3 Further studies by Petroff and McCollough confirmed that this was important in the postsurgical nose.12 A full transfixion incision interrupts both mucosal surfaces and medial crural attachments, allowing the tip to settle closer to the face.11 This occurs because when the full transfixion incision is made, the medial crura reach only part way to the base of the columella.4 Hence, the medial crura no longer play as big a role in tip support after the incision is carried past their attachment to the septum. The nasal tip then heals closer to the face because the feet of the medial crura usually settle until they reach the columella base unless additional support is provided.4 This technique has been recognized as a useful method to deproject the nasal tip, either alone or with other procedures to correct mild to moderate degrees of overprojection.
Despite this, there is some controversy whether the full transfixion incision affects nasal tip projection. Beaty, et al. found the placement of transfixion incisions had no effect on tip support in cadavers.6 Furthermore, he agreed with a conclusion by Tebbets that “soft tissue incisions were the scapegoat for the real cuprit-destructive tip shaping”.6,13
Although several studies looking at nasal tip deprojection have included complete transfixion incisions as part of their technique or in cadavers, no study quantified the effect of the full transfixion incision alone on nasal tip deprojection in humans.4,6,12 Also, even though it has been described that patients with certain skin thickness quality may have different results compared to others, there are no studies which have confirmed this experience in nasal tip deprojection.4
Unlike other studies which have measured nasal deprojection pre- and postoperatively, in our study measurements were taken before and immediately after a full transfixion incision was performed. It was felt that this would be useful to look at the cause and effect of one specific maneuver, namely the full transfixion incision. Also, no local anaesthetic was used prior to the measurement. This is important since it has been reported that there is a real increase in projection of the tip by 1.5 mm before the procedure begins with the administration of local anaesthetic and manipulation of the nose.12 All efforts were made to minimally alter or manipulate the nasal anatomy so that true nasal deprojection measurements were performed and the results would not be altered artificially.
We set out to critically assess the impact of the full transfixion incision on nasal tip projection to allow us an objective way to plan nasal tip deprojection surgery. The data in our study supports the concept of the full transfixion incision having a quantitative effect on nasal tip deprojection. The overall mean in nasal tip deprojection in our study was 2.12 mm immediately after the incision was made. This number may be considered small but this measurement is comparable to other studies which found an average of 2.4 mm in tip deprojection, with the incision in combination of other procedures, during the first 6 months following surgery.12
Second, patients were subjectively grouped into different skin thickness types to study if there was a difference in results based on this characteristic. Patients with thin skin had a larger nasal tip deprojection compared to those with medium or thick skin. Although not a large difference between the groups, the results were statistically different. Patients with thin skin are more at risk for postoperative deformities and asymmetries of the tip due to the way thin skin drapes over the new nasal skeleton.4 This will aide in surgical planning for patients with mild to moderate overprojected nasal tips who have thin skin that may reduce the number of maneuvers required to achieve the aesthetic goal.
Conclusions
The study goal to evaluate objectively the effects of the transfixion incision on tip projection was successful. We were able to quantify the effects of the full transfixion incision on nasal tip surgery. Also, we were able to demonstrate that patients with thin skin had a greater reduction in tip projection than patients assessed to have medium or thick skin. We believe that it is an important method of decreasing projection as one of the many tools available to the rhinoplasty surgeon. Also, the graduate approach is important with the least destructive methods to the nasal anatomy employed first.
References
| 1. | Fredricks S. Tripod Resection for “Pinocchio” Nose Deformity. Plast Reconstr Surg 53:531-533, 1974. |
| 2. | Cummings: Otolaryngology-Head and Neck Surgery, ed.3 |
| 3. | Janeke, JB, Wright, WK. Studies on the support of the Nasal Tip. Arch Otolaryng 93:458-464, 1971. |
| 4. | Mc Cullough E, Mangat D. Systemic Approach to Correction of the Nasal Tip in Rhinoplasty. Arch Otolaryngol Head Neck Surg 107:12-16, 1981. |
| 5. | Anderson, JR. A Reasoned Approach to Nasal Base Surgery. Arch Otolaryng 110:349-358, 1984. |
| 6. | Beaty MM, Dyer WK, Shawl MW. The Quantification of Surgical Changes in Nasal Tip Support. Arch Facial Plast Surg 4:82-91, 2002. |
| 7. | Anderson JR, Ries WR. Rhinoplasty: Emphasizing the External Approach. New York, NY: Thieme-Stratton Inc; 1986. |
| 8. | Adams WP Jr., Rohrich RJ, Hollier LH, Minoli J, Thornton LK, Gyimesi I. Anatomic Basis and Clinical Implications for Nasal Tip Support in Open vs Closed Rhinoplasty. Plast Reconstr Surg 103(1):255-261, 1999. |
| 9. | Simons R, Nasal Tip Projection, Ptosis and Supratip Thickening. Ear Nose Throat J 61:454-455, 1982. |
| 10. | Crumley RL, Lanser M. Quantitative Analysis of Nasal Tip Projection. Laryngoscope 98:202-208, 1988. |
| 11. | Papel ID, Mabrie DC. Deprojecting the Nasal Profile. Otolaryngol Clin North America 32(1):65-87, 1999. |
| 12. | Petroff MA, McCollough EG, Hom D, Anderson JR. Nasal Tip Projection: Quantitative Changes Following Rhinoplasty. Ach Otoloaryngol Head Neck Surg 117:783-788, 1991. |
| 13. | Tebbets JB. Primary Rhinoplasty: A New Approach to the Logic and the Techniques. St. Louis, Mo: Mosby-Year Book Inc., 1998. |
| Table 1. Reduction of Nasal Tip Projection | ||||||||||||||||
|
| Table 2. Post hoc test comparing results of skin thickness quality. | |||||||||||||||||||||||||
|
|||||||||||||||||||||||||